文章信息
- 刘欣然, 马晶茹
- LIU Xinran, MA Jingru
- 急性冠脉综合征患者中性粒细胞百分比与白蛋白比值与冠状动脉病变程度及预后的相关性
- Correlation between neutrophil percentage-to-albumin ratio and coronary lesion severity and prognosis in patients with acute coronary syndrome
- 中国医科大学学报, 2025, 54(10): 902-906, 913
- Journal of China Medical University, 2025, 54(10): 902-906, 913
-
文章历史
- 收稿日期:2025-06-05
- 网络出版时间:2025-10-15 16:03:15
急性冠脉综合征(acute coronary syndrome,ACS)通常由冠状动脉粥样硬化性斑块破裂引起,而炎症在斑块的形成及发展、破裂中发挥着重要作用[1-2]。因此,为了更好地防治ACS,炎症评价指标成为研究热点[3]。其中,中性粒细胞百分比与白蛋白比值(neutrophil percentage-to-albumin ratio,NPAR)是一个新的反映炎症水平及营养状况的综合性炎症指标[4]。研究显示,NPAR对心房颤动[5]、心力衰竭[6]、心源性休克[7]等心血管疾病具有较好的预测价值。但关于NPAR与ACS的研究较少,因此,本研究拟观察NPAR与ACS患者冠状动脉病变严重程度的关系,并评估其对短期内发生主要不良心血管事件(major adverse cardiovascular event,MACE)的预测价值。
1 材料与方法 1.1 研究对象选择2020年1月至2023年12月于沈阳医学院附属第二医院就诊并进行冠状动脉造影(coronary angiography,CAG)的初诊ACS患者345例。所有患者均符合《2023 ESC急性冠脉综合征治疗指南》 [8]中的ACS诊断标准。其中,女103例,男242例。纳入标准:年龄≥18岁;初发;进行CAG检查;临床资料、生化指标、1年随访资料完整,均有明确随访结果;CAG检查及介入治疗均由同一组介入医生完成。排除标准:合并其他重大疾病(恶性肿瘤、活动性感染性疾病、全身性炎症性疾病);慢性终末期器官功能不全(慢性肾衰竭、肝功能严重异常、慢性阻塞性肺疾病);急性干扰因素(1个月内有严重外伤、外科手术或大出血病史);入院前接受过糖皮质激素、免疫抑制剂或抗生素治疗。本研究经沈阳医学院附属第二医院医学伦理委员会批准(2024-沈医二院伦理-011)。所有研究对象签署知情同意书。
1.2 方法 1.2.1 资料收集从我院计算机管理系统中提取研究对象的临床资料。计算复合型指标,包括NPAR、中性粒细胞与淋巴细胞比值(neutrophil-to-lymphocyte ratio,NLR)、血小板与淋巴细胞比值(platelet-to-lymphocyte ratio,PLR)、系统性免疫炎症指数(systemic immune-inflammation index,SII,即血小板计数×中性粒细胞计数/淋巴细胞计数),以及红细胞分布宽度与血小板比值(red blood cell distribution width-to-platelet ratio,RPR)、Gensini评分(Gensini score,GS,即病变节段的狭窄评分×病灶部位系数之和)。
根据随访资料,判定患者1年内是否发生MACE。MACE定义为心血管死亡、再发非致死性心肌梗死、心力衰竭、严重恶性心律失常以及非计划内再次血运重建。
1.2.2 患者分组根据NPAR值,采用三分位法将患者分为低NPAR组(NPAR < 1.58,n = 115)、中NPAR组(NPAR 1.58~ < 1.88,n = 115)、高NPAR组(NPAR≥1.88,n = 115)。
1.3 统计学分析采用SPSS 29.0统计软件进行数据分析。计量资料用M(P25~P75)表示,采用单因素方差分析进行比较;计数资料用率(%)表示,采用χ2检验进行比较。采用Spearman相关性检验分析相关性。采用logistic回归评价MACE发生的风险。绘制受试者操作特征(receiver operating characteristic,ROC)曲线,计算曲线下面积(area under the curve,AUC)。所有检验为双侧检验,P < 0.05为差异有统计学意义。
2 结果 2.1 各组ACS患者基线特征比较3组患者体重指数(body mass index,BMI)、白细胞(white blood cell,WBC)计数、淋巴细胞(lymphocyte,LYM)计数、中性粒细胞(neutrophil,NEU)计数、血小板(platelet,PLT)计数、红细胞分布宽度(red blood cell distribution width,RDW)、肌钙蛋白T(cardiac troponin T,cTnT)、N末端脑钠肽前体(N-terminal pro-brain natriuretic peptide,NT-proBNP)、肌酸激酶同工酶(creatine kinase myocardial band,CK-MB)、高密度脂蛋白胆固醇(high-density lipoprotein cholesterol,HDL-C)、空腹血糖(fasting blood glucose,FBG)、中性粒细胞百分比(neutrophil percentage,NE%)、白蛋白(albumin,ALB)、NLR、PLR、SII、RPR比较,差异有统计学意义(P < 0.05)。3组年龄、性别(男性)、高血压病史、2型糖尿病史、低密度脂蛋白胆固醇(low-density lipoprotein cholesterol,LDL-C)及甘油三酯(triglycerides,TG)比较,差异无统计学意义(P > 0.05)。见表 1。
| Item | Low NPAR group(n = 115) | Medium NPAR group(n = 115) | High NPAR group(n = 115) | H/χ2/F | P |
| Age(year) | 65.0(58.0-71.5) | 64.0(57.0-70.5) | 64.0(57.0-72.0) | 0.34 | 0.844 |
| Male [n(%)] | 75(65.2) | 86(74.8) | 81(70.4) | 2.52 | 0.284 |
| BMI(kg/m2) | 25.06(19.72-32.87) | 25.15(19.05-32.87) | 26.70(18.78-36.05) | 17.13 | < 0.001 |
| History of hypertension [n(%)] | 66(57.10) | 72(61.00) | 67(60.00) | 0.75 | 0.689 |
| History of diabetes [n(%)] | 37(32.40) | 48(38.10) | 41(39.00) | 2.33 | 0.313 |
| WBC(×109/L) | 7.28(6.00-8.16) | 9.01(8.58-10.94) | 10.33(8.19-12.28) | 67.56 | < 0.001 |
| LYM(×109/L) | 1.96(1.58-2.49) | 1.61(1.32-2.18) | 1.26(0.94-1.67) | 68.41 | < 0.001 |
| NEU(×109/L) | 4.12(3.61-5.39) | 6.28(4.75-7.87) | 7.83(6.20-9.92) | 121.88 | < 0.001 |
| PLT(×109/L) | 201(176.50-228.50) | 223(179.00-251.00) | 223(198.50-266.50) | 19.21 | < 0.001 |
| RDW(%) | 12.9(12.50-13.41) | 12.9(12.50-13.30) | 13.1(12.60-13.70) | 7.13 | 0.028 |
| cTnT(ng/mL) | 0.205(0.310-1.225) | 0.220(0.036-1.033) | 0.400(0.142-1.375) | 10.15 | 0.006 |
| NT-proBNP(pg/mL) | 587.90(262.80-809.00) | 609.05(262.60-1 418.45) | 765.30(315.40-2 219.25) | 9.96 | 0.007 |
| CK-MB(μg/L) | 10.4(7.35-21.30) | 17.5(10.80-57.85) | 23.8(11.85-101.00) | 34.02 | < 0.001 |
| LDL-C(mmol/L) | 2.82(2.15-3.47) | 2.49(2.08-3.25) | 2.76(2.35-3.32) | 3.12 | 0.209 |
| HDL-C(mmol/L) | 1.11(0.94-1.32) | 0.99(0.83-1.20) | 1.02(0.88-1.21) | 7.68 | 0.022 |
| TG(mmol/L) | 4.63(4.15-5.25) | 4.35(3.74-4.97) | 4.51(3.92-5.12) | 5.12 | 0.077 |
| FBG(mmol/L) | 5.89(5.33-7.28) | 6.99(5.53-8.47) | 6.33(5.69-10.10) | 9.54 | 0.008 |
| NE% | 59.67(56.21-59.52) | 71.91(67.41-75.85) | 79.19(74.23-83.52) | 158.14 | < 0.001 |
| ALB(g/L) | 43.2(40.80-45.95) | 41.2(39.15-43.40) | 36.8(33.65-39.20) | 144.48 | < 0.001 |
| NLR | 2.03(1.69-2.65) | 3.73(2.78-4.58) | 6.06(4.52-8.67) | 174.17 | < 0.001 |
| PLR | 102.13(80.46-134.09) | 124.43(97.12-168.98) | 180.91(133.08-255.82) | 90.68 | < 0.001 |
| SII | 411.90(318.31-540.83) | 798.08(566.53-1 067.98) | 1 372.74(980.75-2 174.20) | 173.69 | < 0.001 |
| RPR | 0.066(0.055-0.075) | 0.056(0.052-0.073) | 0.060(0.047-0.068) | 12.93 | 0.001 |
| BMI,body mass index;WBC,white blood cell;LYM,lymphocyte;NEU,neutrophil;PLT,platelet;RDW,red blood cell distribution width;cTnT,cardiac troponin T;NT-proBNP,N-terminal pro-brain natriuretic peptide;CK-MB,creatine kinase myocardial band;LDL-C,low-density lipoprotein cholesterol;HDL-C,high-density lipoprotein cholesterol;TG,triglyceride;FBG,fasting blood glucose;NE%,neutrophil percentage;ALB,albumin;NLR,neutrophil-to-lymphocyte ratio;PLR,platelet-to-lymphocyte ratio;SII,systemic immune-inflammation index;RPR,red blood cell distribution width-to-platelet ratio. | |||||
2.2 加重冠状动脉病变的危险因素
将基线资料中P < 0.05的因素及NPAR作为自变量,采用Spearman相关性检验分析其与GS的相关性,结果显示,共13个变量与GS存在相关性,其中呈正相关的因素包括NPAR、BMI、WBC、NEU、RDW、NT-proBNP、FBG、NE%、NLR、PLR、SII,呈负相关的因素包括ALB和LYM。其他变量差异无统计学意义(P > 0.05)。多元线性回归分析显示,NPAR、年龄、WBC、SII和BMI是冠状动脉病变加重的独立危险因素。见表 2。
| Item | β | SE | t | 95%CI | P | |
| Lower limit | Upper limit | |||||
| Age | 6.137 | 2.053 | 2.989 | 2.098 | 10.176 | 0.003 |
| Male | 1.966 | 1.941 | 1.013 | -1.853 | 5.784 | 0.312 |
| NPAR | 12.744 | 4.014 | 3.175 | 4.847 | 20.640 | 0.002 |
| NLR | 2.178 | 2.881 | 0.756 | -3.489 | 7.844 | 0.450 |
| SII | 6.104 | 2.040 | 2.992 | 2.106 | 10.102 | 0.002 |
| NE% | 0.942 | 2.345 | 0.402 | -3.671 | 5.556 | 0.688 |
| ALB | -2.974 | 3.075 | -0.967 | -9.022 | 3.074 | 0.334 |
| WBC | 5.327 | 2.358 | 2.259 | 0.688 | 9.966 | 0.025 |
| LYM | 0.068 | 1.935 | 0.035 | -3.739 | 3.875 | 0.972 |
| BMI | 5.848 | 1.872 | 3.124 | 2.165 | 9.531 | 0.002 |
| FBG | 1.681 | 1.864 | 0.902 | -1.986 | 5.349 | 0.368 |
| NT-proBNP | 0.831 | 1.865 | 0.445 | -2.838 | 4.500 | 0.656 |
2.3 3组患者MACE发生情况比较
根据随访记录,将随访时间分为4个时间段(≤30 d、> 30~90 d、> 90~180 d、> 180 d~1年),比较低、中、高NPAR组CAG术后不同时间段内MACE的发生情况。结果显示,在术后≤30 d及 > 30~90 d期间,高NPAR组MACE发生率(13.91%,10.43%)显著高于中NPAR组(3.48%,3.48%)和低NPAR组(1.74%,3.48%),差异有统计学意义(P < 0.05)。以低NPAR组为基准,剔除年龄和性别2个混杂因素后,将高血压病史、2型糖尿病史、BMI、NT-proBNP、SII、LDL-C、FBG、NLR及支架数量作为协变量,建立逻辑回归模型,分析不同NPAR水平与短期(≤30 d、> 30~90 d)内MACE发生风险的相关性。结果显示,在术后≤30 d内,NPAR水平增高是发生MACE的独立危险因素。见表 3。
| MACE onset time | β | OR | 95%CI | P | |
| Lower limit | Upper limit | ||||
| ≤30 d | |||||
| Low NPAR group | - | 1.00 | - | - | - |
| Medium NPAR group | 0.313 | 1.37 | 0.600 | 3.127 | 0.457 |
| High NPAR group | 0.891 | 2.44 | 1.150 | 5.135 | 0.020 |
| > 30-90 d | |||||
| Low NPAR group | - | 1.00 | - | - | - |
| Medium NPAR group | 0.069 | 1.07 | -0.510 | 2.251 | 0.855 |
| High NPAR group | 0.417 | 1.52 | -0.764 | 3.014 | 0.233 |
| The low NPAR group is used as the reference group and its OR value is set to 1 by defautt. | |||||
2.4 NPAR对短期内(30 d内)MACE的预测价值
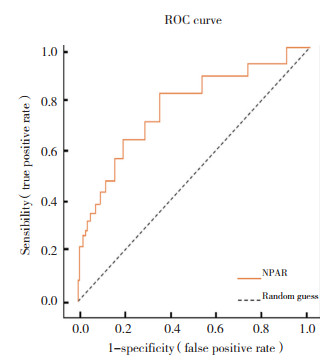
以NPAR作为预测变量,ACS患者30 d内MACE发生情况为状态变量,构建ROC曲线模型,计算灵敏度、特异度和最佳截断值。结果显示,当NPAR > 2.013,ACS患者30 d内MACE发生率的AUC为0.811,灵敏度为70.04%,特异度为81.42%。见图 1。
|
| 图 1 NPAR预测MACE的ROC曲线 Fig.1 ROC curves of NPAR for predicting MACE |
3 讨论
ACS是冠状动脉血液流量急剧减少或中断引发的心肌急剧缺血导致的疾病[9],以起病急骤、变化复杂、病死率高为特点。寻找方便、快捷、敏感的指标对判定ACS患者病情及预后具有重要意义[8, 10]。
近年的研究[11-12]发现,炎症细胞在促进冠状动脉斑块破裂及血栓形成过程中具有重要作用。2019年,NPAR作为一种复合型炎症指标被首次提出[13],创新性地整合了炎症反应与营养状态2个重要生理学参数。相比于单一的炎症指标,NPAR预测心血管疾病发病风险更准确。HUANG等[14]研究发现,较高NPAR水平与心血管病高风险密切相关,NPAR每增高1个单位,心血管事件发生率增高3%。SERHATLIOGLU等[15]的研究显示,高NPAR水平与冠状动脉旁路移植术后早期心房颤动的发生显著相关,可预测术后早发心房颤动。本研究通过对ACS患者临床基线资料比较发现,高NPAR组cTnT、CK-MB水平高于低NPAR组和中NPAR组(P < 0.05)。提示NPAR水平越高,炎症反应越强,氧化应激也随之增强,心肌损伤加重[16]。此外,本研究结果显示,NPAR与LDL-C无相关性,与HDL-C有相关性。这可能由于LDL-C的核心致病机制是通过胆固醇沉积-泡沫细胞形成驱动冠状动脉粥样斑块形成[17-18],而NPAR反映的是粥样斑块破裂后的炎症反应或血栓风险[19],两者分别作用于动脉粥样硬化的不同阶段,在相互作用机制上无直接因果链。HDL-C具有抗炎、抗氧化等心血管保护作用,NPAR升高所致炎症状态会影响HDL-C的代谢和功能,因此,NPAR与HDL-C之间呈现相关性。本研究还发现,NPAR与GS呈正相关,且相关性优于单一炎症指标和其他炎症复合指标(包括NLR、PLR、SII),且NPAR是冠状动脉病变加重的独立危险因素。
本研究还进一步分析了NPAR水平与ACS患者随访不同时间段MACE发生率的关系。结果发现,随访30 d内,高NPAR组的MACE发生率显著高于中、低NPAR组,且高NPAR组MACE发生率为低NPAR组的2.44倍,表明高水平NPAR的ACS患者在短期内更容易出现不良心血管事件,其潜在机制可能是在急性期内,急性炎症损伤与全身营养-稳态失衡以多重分子通路形成正反馈,促进了MACE的发生[20-21]。在ACS早期,白细胞介素-6、白细胞介素-1β等促炎性细胞因子通过JAK-STAT通路激活肝脏急性期反应,抑制肝脏ALB的转录[22],导致血清ALB水平下降,且其降幅与NEU成反比[21]。同时,NE释放的酶类会破坏血管内皮的紧密连接[23],导致ALB外漏,造成低白蛋白血症,这一病理状态不仅阻碍血管的修复进程,还增强了PLT的敏感性,极大地提高了患者早期MACE的发生风险。而在随访晚期,机体可以依靠抗炎、修复、代谢调整等多种途径,部分抵偿上述影响[24]。故“急性炎症-营养失衡”正反馈循环通路极可能是ACS患者早期MACE风险升高的关键因素。本研究通过绘制ROC曲线发现,当NPAR > 2.013时,对30 d内MACE发生率有较好的预测价值。
综上所述,NPAR这一反映炎症和免疫状态的生物标志物简便易得,可以提高ACS患者的危险分层准确性和预后评估能力,有助于进一步制定个体化康复及随访计划。但本研究是单中心回顾性研究,在研究样本量、涉及范围等方面有一定的局限性,有待后期开展多中心、大样本的前瞻性队列研究,为ACS的早期诊断和精准化管理提供更坚实的科学依据。
| [1] |
KORKMAZ-ICÖZ S, SZABÓ G, GIELDON A, et al. Protective effects of neutrophil serine protease inhibition against ischemia-reperfusion injury in lung or heart transplantation[J]. FEBS J, 2025. DOI:10.1111/febs.17411 |
| [2] |
HUNTERMANN R, PERES DE OLIVEIRA J, BARBOSA LM, et al. Colchicine in acute coronary syndromes: a systematic review and meta-analysis of randomised controlled trials[J]. Heart, 2025, heartjnl-2025-325826. DOI:10.1136/heartjnl-2025-325826 |
| [3] |
LAKSHMIPRIYA T, GOPINATH SCB, CHEN Y, et al. Current attainments on nanobiosensors for diagnosing atherosclerosis biomarkers[J]. Curr Med Chem, 2025. DOI:10.2174/0109298673360990250408111013 |
| [4] |
SEYDEL GS, GUNTURK I, AKKAYA H, et al. The relationship between the new inflammatory markers and disease severity in patients with acute coronary syndrome[J]. Acta Cardiol, 2024, 79(7): 778-786. DOI:10.1080/00015385.2024.2403933 |
| [5] |
XU YX, LIN ZH, ZHU CX, et al. The neutrophil percentage-to-albumin ratio is associated with all-cause mortality in patients with atrial fibrillation: a retrospective study[J]. J Inflamm Res, 2023, 16: 691-700. DOI:10.2147/JIR.S394536 |
| [6] |
WANG X, ZHANG Y, WANG YX, et al. The neutrophil percentage-to-albumin ratio is associated with all-cause mortality in patients with chronic heart failure[J]. BMC Cardiovasc Disord, 2023, 23(1): 568. DOI:10.1186/s12872-023-03472-9 |
| [7] |
YU Y, LIU Y, LING XY, et al. The neutrophil percentage-to-albumin ratio as a new predictor of all-cause mortality in patients with cardiogenic shock[J]. Biomed Res Int, 2020, 2020: 7458451. DOI:10.1155/2020/7458451 |
| [8] |
BUSKE M, FEISTRITZER HJ, JOBS A, et al. Management of acute coronary syndrome: esc guidelines 2023[J]. Herz, 2024, 49(1): 5-14. DOI:10.1007/s00059-023-05222-1 |
| [9] |
ROMERO NOBOA ME, ARORA S, KANSAL P, et al. Analysis of takayasu's arteritis as a risk factor for acute coronary syndrome[J]. Am J Med Open, 2025, 13: 100096. DOI:10.1016/j.ajmo.2025.100096 |
| [10] |
JIANG SH, LIU SY, XIAO GE, et al. Atherogenic index of plasma and the clinical outcome of patients with acute coronary syndrome: a meta-analysis[J]. Ann Med, 2025, 57(1): 2442532. DOI:10.1080/07853890.2024.2442532 |
| [11] |
TIMPAU AS, MIFTODE EG, COSTACHE-ENACHE Ⅱ, et al. Integrating the interleukins in the biomarker panel for the diagnosis and prognosis of patients with acute coronary syndromes: unraveling a multifaceted conundrum[J]. Diagnostics, 2025, 15(10): 1211. DOI:10.3390/diagnostics15101211 |
| [12] |
SONG KX, YAO WJ, YAN HH, et al. Associations between the platelet lymphocyte ratio and albumin with plaque calcification in patients with acute coronary syndrome: an optical coherence tomography study[J]. Rev Cardiovasc Med, 2025, 26(4): 28167. DOI:10.31083/RCM28167 |
| [13] |
CUI HH, DING XS, LI WP, et al. The neutrophil percentage to albumin ratio as a new predictor of in-hospital mortality in patients with ST-segment elevation myocardial infarction[J]. Med Sci Monit, 2019, 25: 7845-7852. DOI:10.12659/MSM.917987 |
| [14] |
HUANG XF, ZHANG YQ, HAO WT, et al. The association between neutrophil percentage-to-albumin ratio and cardiovascular disease: evidence from a cross-sectional study[J]. Front Cardiovasc Med, 2025, 12: 1557507. DOI:10.3389/fcvm.2025.1557507 |
| [15] |
SERHATLIOGLU F, YILMAZ Y, BARAN O, et al. Inflammatory markers and postoperative new-onset atrial fibrillation: prognostic predictions of neutrophil percent to albumin ratio in patients with CABG[J]. Diagnostics, 2025, 15(6): 741. DOI:10.3390/diagnostics15060741 |
| [16] |
HAN DZ, WU LL, ZHOU HB, et al. Neutrophil percentage-to-albumin ratio and the risk of all-cause and cardiovascular mortality: a 20-year follow-up cohort study of 36, 428 US adults[J]. BMC Public Health, 2025, 25(1): 1483. DOI:10.1186/s12889-025-22764-7 |
| [17] |
WHITMORE K, ZHOU Z, RYAN JDM, et al. Influence of repeated plaque visualization on cardiovascular risk reduction after 3 years: a randomized controlled trial[J]. Eur J Prev Cardiol, 2025, 32(7): 596-605. DOI:10.1093/eurjpc/zwae026 |
| [18] |
BHARGAVA P, DINH D, TERAMAYI F, et al. Selective removal of 7-ketocholesterol by a novel atherosclerosis therapeutic candidate reverts foam cells to a macrophage-like phenotype[J]. Atherosclerosis, 2025, 119217. DOI:10.1016/j.atherosclerosis.2025.119217 |
| [19] |
XU MX, ZHAI Q, WEI B, et al. Higher neutrophil-percentage-to-albumin ratio was associated with poor outcome in endovascular thrombectomy patients[J]. Ther Clin Risk Manag, 2025, 21: 565-573. DOI:10.2147/TCRM.S519263 |
| [20] |
PÉREZ-OLIVARES L, SOEHNLEIN O. Contemporary lifestyle and neutrophil extracellular traps: an emerging link in atherosclerosis disease[J]. Cells, 2021, 10(8): 1985. DOI:10.3390/cells10081985 |
| [21] |
ECKART A, STRUJA T, KUTZ A, et al. Relationship of nutritional status, inflammation, and serum albumin levels during acute illness: a prospective study[J]. Am J Med, 2020, 133(6): 713-722. e7. DOI:10.1016/j.amjmed.2019.10.031 |
| [22] |
YANG XF, MA YP, CHEN X, et al. Mechanisms of neutrophil extracellular trap in chronic inflammation of endothelium in atherosclerosis[J]. Life Sci, 2023, 328: 121867. DOI:10.1016/j.lfs.2023.121867 |
| [23] |
ZHANG ZY, WANG YX, LI T, et al. NETosis in myocardial ischemia-reperfusion injury: from mechanisms to therapies (review)[J]. Biomed Rep, 2025, 23(1): 113. DOI:10.3892/br.2025.1991 |
| [24] |
WANG HM, LIU ZF, SHAO JJ, et al. Immune and inflammation in acute coronary syndrome: molecular mechanisms and therapeutic implications[J]. J Immunol Res, 2020, 2020: 4904217. DOI:10.1155/2020/4904217 |
 2025, Vol. 54
2025, Vol. 54