Acute pulmonary embolism (PE) is a life-threatening cardiovascular emergency with high mortality rate[1]. only 7% of the patients who died early were correctly diagnosed with PE before death[2]. Patients who received heparin in the emergency room had lower rate in-hospital mortality and 30-day mortality[3]. Current guideline recommends in patients with high or intermediate clinical probability for PE parenteral anticoagulation should be initiated while waiting the results of diagnostic tests[4]. Can anticoagulation be more rapid and efficacious? Initial intrvenous injection(Ⅳ) loading dose of 30 mg enoxaparin was recommended for the treatment of acute coronary syndrome(ACS) because it allows immediately reaching to therapeutic and steady-state conditions, and it's safe and more efficacious than unfractionated heparin (UFH)[5, 6]. In the acute phase of PE, initial Ⅳ enoxaparin was not reported as far as we know. We present a case of acute PE which initially was falsely diagnosed and treated as ACS, while having positive results.
Case ReportA 24-year-old man presented to emergency department in May 2014, with 2-hour chest pain and dyspnea. Medical history included recently diagnosed advanced testicular cancer, but we did not know until half an hour later when he could tell.
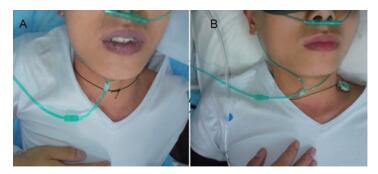
At presentation, the patient had a heart rate of 140 beats/min, a respiratory rate of 50 /min, a peripheral oxygen saturation of 50% and a blood pressure of 70/40 mmHg. He was markedly cyanotic (Figure 1A). Auscultation of the lungs was clear. ECG showed sinus tachycardia.
|
Figure 1 A, patient was markedly cyanotic even with high oxygen supply; B, 1 hour after treatment, cyanosis was gone. |
He was treated with supplemental oxygen, oral aspirin 300 mg and enoxaparin was administered immediately as a 30mg Ⅳ bolus followed by 1 mg/kg subcutaneously, for a presumed diagnoses of ACS.
The patient's blood pressure was improved rapidly: 1 hour later, the heart rate was 124 beats/min, blood pressure 95/65 mmHg, respiratory rate 30 /min and oxygen saturation 95% on supplemental oxygen. And cyanotic disappeared (Figure 1B). A second ECG revealed sinus tachycardia with no ST-T wave abnormalities. The diagnosis of pulmonary embolism was made on pulmonary computed tomographic angiography (PCTA) (Figure 2). Subcutaneous enoxaparin 1 mg/kg continued over the next 12 hours. A second PCTA undertaken 30 hours later showed a substantial reduction in the volume of pulmonary emboli and restoration of right pulmonary blood flow (Figure 3). He made a full recovery and was discharged with a plan for long-term warfarin therapy.
|
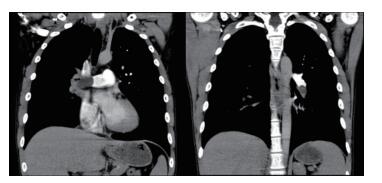
Figure 2 PCTA at 2 hours after Ⅳ enoxaparin showed right trunk and left pulmonary artery embolism. |
|
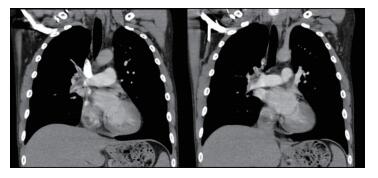
Figure 3 PCTA at 32 hours after Ⅳ enoxaparin showed reduction in the volume of pulmonary emboli and restoration of right pulmonary blood flow. |
In patients with acute PE, anticoagulation can objectively prevent early death[7]. In this case, patient's vital signs were stabilized quickly after anticoagulation. In the following 30 hours, PCTA images showed reduction in the volume of pulmonary emboli and restoration of pulmonary blood flow. Subcutaneous low-molecular-weight heparin (LMWH) is preferred over UFH for initial anticoagulation in PE without shock or hypotension[4].Peak values of anti-Xa activity were measured few hours after subcutaneous LMWH[8]. Enoxaparin as a widely used LWMH, Ⅳ loading dose allows immediately to reach therapeutic anti-Xa levels and steady-state conditions. Early anticoagulation is associated with reduced mortality for acute pulmonary embolism[3].Compare with subcutaneous alone, a loading dose earned more efficacious anticoagulation in the first few hours. And this may further reduce mortality for acute pulmonary embolism.
UFH is recommended in this situation when primary reperfusion is considered[4]. Enoxaparin has been proven to be more efficacious than UFH when a loading Ⅳ dose was initiated[9, 10].A more efficacious anticoagulation could offer quicker and better opportunity to stabilize patients' hemodynamic status. Labèque et al reported Ⅳ enoxaparin administration before primary angioplasty for ST-elevation acute myocardial infarction, which was associated with a high percentage of initial TIMI 3 flow in the infarct related artery[11]. After Ⅳ loading dose of enoxaparin, anti-IIa and aPTT are higher than steady-state levels, but only for a few hours following the initial loading dose[12]. If initial anticoagulation to start fibrinolysis need few hours, then loading dose of enoxaparin would have little influence to fibrinolysis[3]. In patients received fibrinolysis for ST-elevation myocardial infarction, treatment with enoxaparin is superior than that with UFH for 48 hours but is associated with an increase in major bleeding episodes[9]. Increase bleeding chance should be considered when acute PE patients treated with thrombolytic and enoxaparin. Two RCTs have investigated the efficacy and side effects of half-dose alteplase in predominantly sub massive PE[13, 14].Equal efficiency with less hemorrhage was seen when compared with standard-dose alteplase. When Ⅳ loading dose enoxaparin had been administered, half-dose alteplase in PE with shock or hypotension is an option for some patients.This case indicates that treating acute PE with Ⅳ bolus enoxaparin could be a reasonable treatment option which worth further study.
| [1] |
Kearon C. Natural history of venous thromboembolism[J]. Circulation, 2001, 01(01): 27-37. |
| [2] |
Cohen A T, Agnelli G, Anderson F A, et al. Venous thromboembolism (VTE) in Europe. The number of VTE events and associated morbidity and mortality[J]. Thromb Haemost, 2007, 98(4): 756-764. |
| [3] |
Smith S B, Geske JBMaguire J M, Zane N A, et al. Early anticoagulation is associated with reduced mortality for acute pulmonary embolism[J]. . Journal of Emergency Medicine, 2010, 39(5): 712-712. |
| [4] |
Konstantinides SV, Torbicki A, Agnelli G, et al. 2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism[J]. Eur Heart J, 2014, 35(43): 3069-3069. |
| [5] |
Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ACC Guideline for the Management of Patients with Non-ST-Elevation Acute Coronary Syndromes:A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines[J]. J Am Coll Cardiol, 2014, 64(24): 139-228. DOI:10.1016/j.jacc.2014.09.017 |
| [6] |
Steg PG, James SK, Atar D, et al. ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation[J]. Eur Heart J, 2012, 33(20): 2569-2619. DOI:10.1093/eurheartj/ehs215 |
| [7] |
Kline JA1, Hernandez-Nino J, Jones AE, et al. Prospective study of the clinical features and outcomes of emergency department patients with delayed diagnosis of pulmonary embolism[J]. Acad Emerg Med, 2007, 14(7): 592-598. DOI:10.1197/j.aem.2007.03.1356 |
| [8] |
Samama MM, Poller L. Contemporary laboratory monitoring of low molecular weight heparins[J]. Clin Lab Med, 1995, 15(1): 119-123. DOI:10.1016/S0272-2712(18)30347-0 |
| [9] |
Antman EM, Morrow DA, McCabe CH, et al. Enoxaparin versus unfractionated heparin with fibrinolysis for ST-elevation myocardial infarction[J]. NEJM, 2006, 354: 1477-1488. DOI:10.1056/NEJMoa060898 |
| [10] |
Silvain J, Beygui F, Barthélémy O, et al. Efficacy and safety of enoxaparin versus unfractionated heparin during percutaneous coronary intervention:systematic review and meta-analysis[J]. BMJ, 2012, 3: 344-553. |
| [11] |
Labèque JN, Ja s C, Dubos O, et al. Prehospital Administration of Enoxaparin Before Primary Angioplasty for ST-Elevation Acute Myocardial Infarction[J]. Catheter Cardiovasc Interv, 2006, 67(2): 207-213. DOI:10.1002/(ISSN)1522-726X |
| [12] |
Philippe Grosjean, Marie-Laure Ozoux, yvonne Le Roux, et al. Enoxaparin Pharmacokinetics and Pharmacodynamics After intravenous Bolus Administration Alone and at Initiation of a Subcutaneous Dosing Regimen[J]. J Am Coll Cardiol, 2000, 35(2): 1106-1129. |
| [13] |
Sharifi M, Bay C, Skrocki L, et al. Moderate pulmonary embolism treated with thrombolysis (from the 'MOPETT' Trial)[J]. Am J Cardiol, 2013, 111: 273-277. DOI:10.1016/j.amjcard.2012.09.027 |
| [14] |
Wang C, Zhai Z, Yang Y, et al. Efficacy and safety of low dose recombinant tissue-type plasminogen activator for the treatment of acute pulmonary thromboembolism:a randomized, multicenter, controlled trial[J]. Chest, 2010, 137: 254-262. DOI:10.1378/chest.09-0765 |
 2018, Vol. 2
2018, Vol. 2

