文章信息
- 赵晶晶, 张汀汀, 刘晓华, 孙纪新, 刘玉环, 岳福娟, 张帆, 曹亚景.
- Zhao Jingjing, Zhang Tingting, Liu Xiaohua, Sun Jixin, Liu Yuhuan, Yue Fujuan, Zhang Fan, Cao Yajing
- 睡眠时间与成年人代谢综合征相关性的Meta分析
- A Meta-analysis on the association between sleep duration and metabolic syndrome in adults
- 中华流行病学杂志, 2020, 41(8): 1272-1279
- Chinese Journal of Epidemiology, 2020, 41(8): 1272-1279
- http://dx.doi.org/10.3760/cma.j.cn112338-20200106-00013
-
文章历史
收稿日期: 2020-01-06
2. 河北省疾病预防控制中心寄生虫防治所, 石家庄 050021;
3. 北京维世达诊所, 北京 100020
2. Hebei Provincial Center for Disease Control and Prevention of Parasite Control, Shijiazhuang 050021, China;
3. Beijing Vista Medical Center, Beijing 100020, China
MS是一组心血管代谢危险因素的集合,包括腹部肥胖、糖代谢异常、血压升高和血脂异常等[1],其中以腹部肥胖和胰岛素抵抗为临床特征。这些危险因素在人群中易感并在个体中聚集。有研究证实,MS可使患2型糖尿病的风险增加5倍,使患心血管疾病的风险增加3倍[2]。尽管没有精确统一的定义,但无可争议的是MS及其危险因素相互作用增加了个体不良心血管疾病结果的风险。近来有研究表明,睡眠时间过长或过短可能与MS风险增加有关[3-5],但是目前研究结论并不一致,为此,本研究将对睡眠时间与成年人MS之间的关系进行定量评估,以期为MS的防治提供科学依据。
材料与方法1.文献检索策略:检索中国知网、万方、PubMed、Embase、Cochrane数据库,检索时间为2019年10月以前已发表的相关文献。英文检索词以“Metabolic Syndrome”“sleep duration”为Mesh主题词,与“Metabolic Syndromes”“Insulin Resistance*”“Dysmetabolic Syndrome X”“Reaven*”“Cardiovascular Syndrome,Metabolic”“sleep duration”等自由词组合,中文检索词为“睡眠”、“代谢综合征”或“胰岛素抵抗”。语言限制为中文和英文。为避免遗漏,另对纳入研究中的参考文献进行手工检索。
2.纳入排除标准:纳入标准:①与睡眠时间和MS有关的观察性研究;②MS定义明确;③有可提取的风险效应值;④研究人群为≥18岁成年人;排除标准:①综述或Meta分析等;②病理机制性研究。
3.数据提取:由2名研究人员独立提取纳入文献中的相关数据。若有分歧,则通过共同商讨或咨询第三人解决。提取信息包括:第一作者、发表年份、研究对象国别、种族、MS诊断标准、年龄、性别、样本量、病例数、暴露测量、测量时段、睡眠时间和MS的风险效应值等。
4.统计学分析:采用Stata 11.0软件对纳入的文献进行Meta分析。横断面研究选用OR值及其95%CI进行描述,队列研究将OR值及HR值近似等于RR值,选用RR值及其95%CI进行描述。长睡眠时间及短睡眠时间按原文中定义,参照睡眠时间一般为6~8 h,否则根据Hamling等[6]研究进行参照组转换。异质性评估采用Q检验,当P>0.1且I2≤50%时采用固定效应模型;反之,则认为存在异质性,采用随机效应模型。采用Egger’s检验和Begg’s检验评价潜在发表偏倚(P<0.05,认为存在发表偏倚),并进行敏感性分析。按研究设计(横断面研究和队列研究)、种族(白种人、亚洲人及黑种人)、性别、年龄组(<60岁和≥60岁)、测量睡眠时段(24 h和夜晚)进行亚组分析。
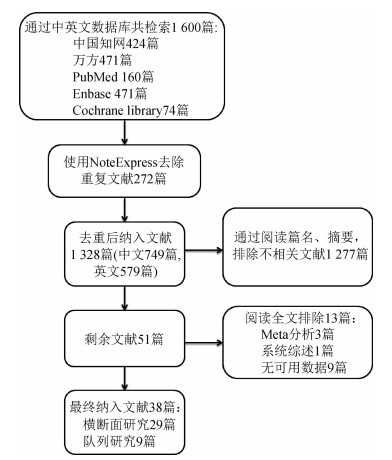
结果1.文献检索结果:通过中国知网、万方、PubMed、Embase及Cochrane library数据库,共检索到1 600篇文献。排除重复、不相关、综述性及无可用数据的文献后,最终纳入38篇文献[3-5, 7-41],中文文献3篇,英文文献35篇。检索流程见图 1。
|
| 图 1 纳入文献筛选流程图 |
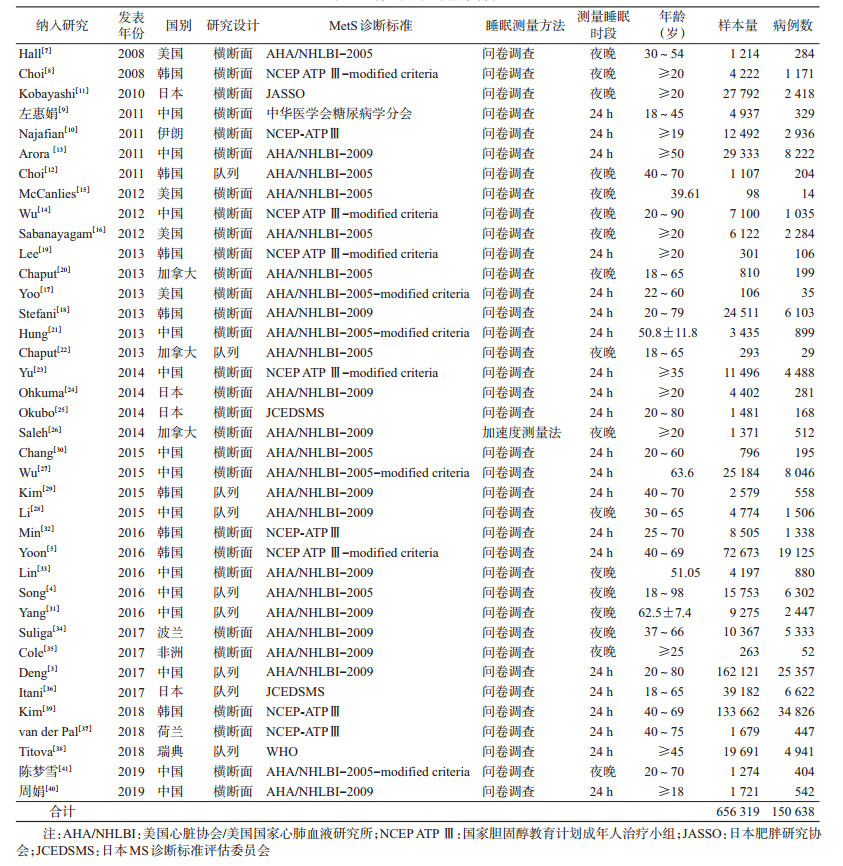
2.纳入文献基本情况:纳入的38篇文献中29篇为横断面研究,其余9篇为队列研究。研究对象均为成年人,共计656 319例,其中MS患者150 638例。MS诊断标准主要采用2005年和2009年美国心脏协会/美国国家心肺血液研究所(American Heart Association/National Heart,Lung,and Blood Institute,AHA/NHLBI),此外还有美国成年人胆固醇教育计划(national cholesterol education program adult treatment panel Ⅲ,NCEP ATPⅢ)、中华医学会糖尿病学分会、日本MS诊断标准评估委员会(Japanese Committee to Evaluate Diagnostic Standards for Metabolic Syndrome,JCEDSMS)、日本肥胖研究协会(Japan Society for the Study of Obesity,JASSO)。17篇测量睡眠时间为夜晚,21篇为24 h。见表 1。
3.睡眠时间与成年人MS关联:
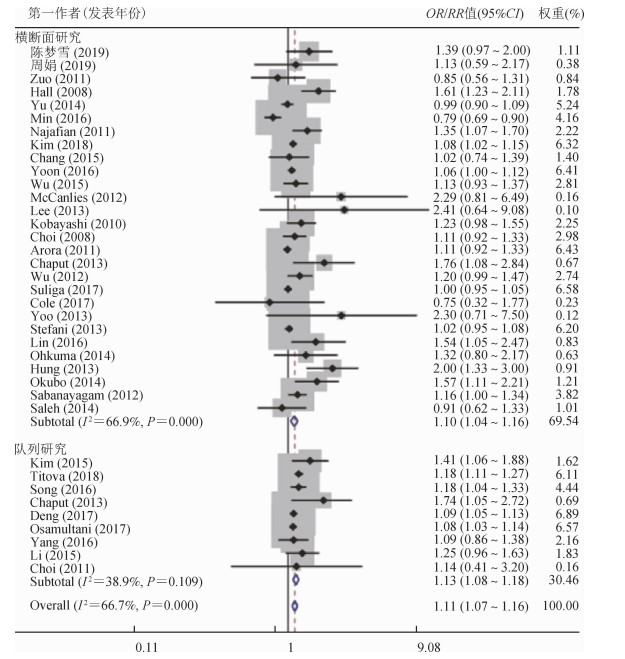
(1)短睡眠时间与MS:研究短睡眠时间与MS关联的文献共37篇,其中横断面研究28篇,队列研究9篇,Q检验结果显示存在异质性(P<0.1,I2=66.7%),故采用随机效应模型,总合并效应量为1.11(95%CI:1.07~1.16),提示相对于正常睡眠组,短睡眠时间可使患MS风险增加11%。横断面研究中,合并OR=1.10(95%CI:1.04~1.16);队列研究中,合并RR=1.13(95%CI:1.08~1.18),队列研究的风险值高于横断面研究。见图 2。
|
| 图 2 短睡眠时间与MS关联的森林图 |
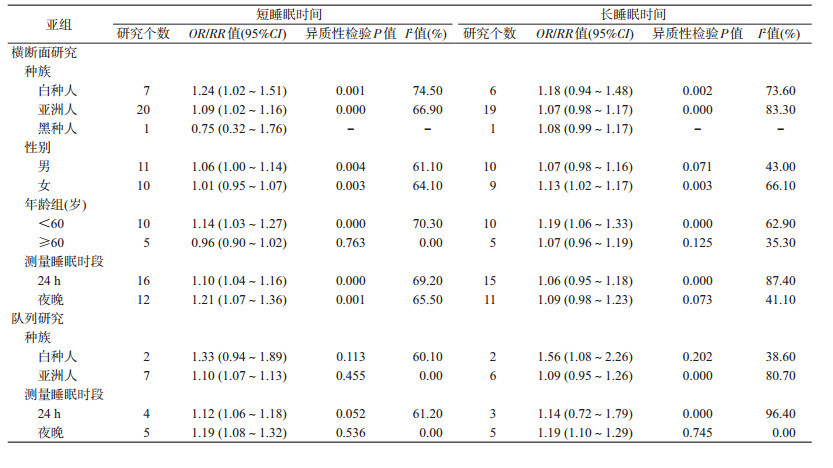
在横断面研究的亚组分析中,短睡眠时间与MS的关联在白种人、亚洲人、男性、<60岁和测量睡眠时段的亚组中更强。在队列研究的亚组分析中,该关联在亚洲人、测量睡眠时段的亚组中更强。见表 2。
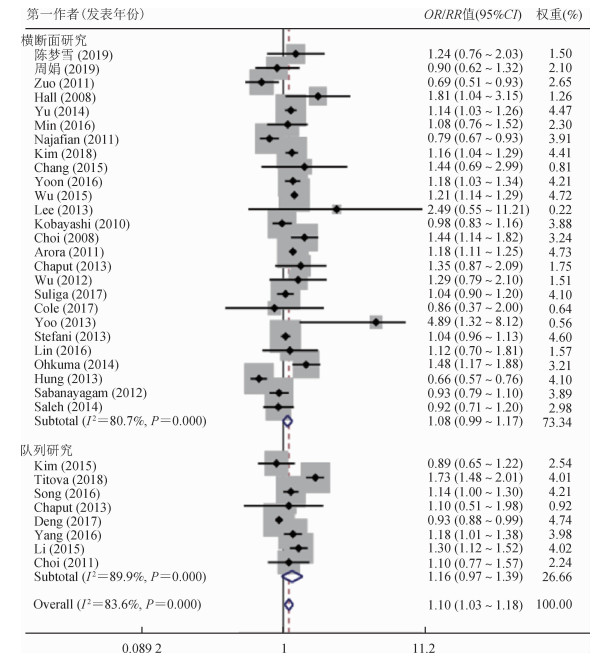
(2)长睡眠时间与MS:研究长睡眠时间与MS关联的文献共34篇,其中横断面研究26篇,队列研究8篇,Q检验结果显示存在异质性(P<0.1,I2=83.6%),故采用随机效应模型,总合并效应量为1.10(95%CI:1.03~1.18),提示相对于正常睡眠组,长睡眠时间可使患MS风险增加10%。但按研究设计分组后并未观察到该结果。横断面研究中,合并OR值为1.08(95%CI:0.99~1.17);队列研究中,合并RR值为1.16(95%CI:0.97~1.39)。见图 3。
|
| 图 3 长睡眠时间与MS关联的森林图 |
在横断面研究的亚组分析中,长睡眠时间与MS的关联在女性和<60岁的亚组中更强。在队列研究的亚组分析中,该关联在白种人和测量睡眠时段为夜晚的亚组中更强。见表 2。
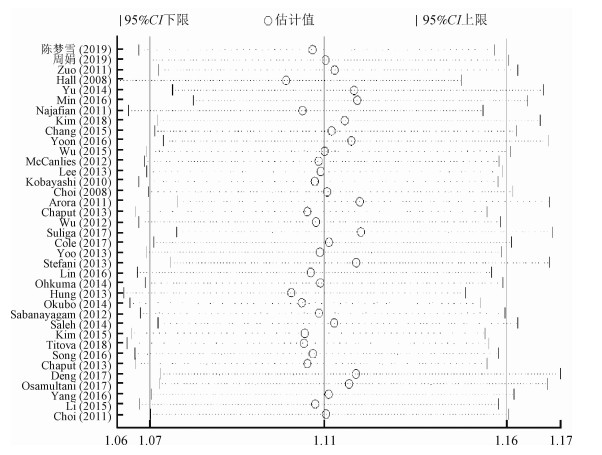
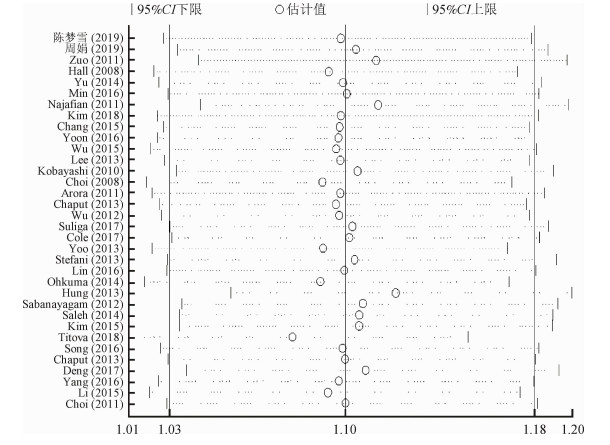
4.发表偏倚及敏感性分析结果:利用睡眠时间与MS关联文献绘制漏斗图,并进行Egger’s检验和Begg’s检验。短睡眠时间中Begg’s检验p=0.07,Egger’s检验p=0.006,提示存在发表偏倚;长睡眠时间中Egger’s检验和Begg’s检验P值分别为0.62和0.63,均>0.05,提示不存在发表偏倚。敏感性分析结果显示,短睡眠时间与长睡眠时间研究中删除任一篇文献对剩余文献合并效应值均无明显影响,证实了本研究最终结果的稳定性。见图 4,5。
|
| 图 4 短睡眠时间与MS研究的敏感性分析 |
|
| 图 5 长睡眠时间与MS研究的敏感性分析 |
睡眠行为可以调节人体激素分泌,对机体代谢也会产生影响。近年来有大量研究表明睡眠过长或过短与MS及其组分如肥胖、糖尿病、高血压等相关[42-44]。本研究表明与正常睡眠相比,短睡眠时间使MS患病风险增加了11%,长睡眠时间使患病风险增加了10%,睡眠时间与MS呈“U”形关联。之前已发表了3项相关荟萃研究[45-47],但纳入的文献主要为横断面研究,队列研究数目有限,本研究在此基础上,又加入了近5年新发表的文献,其中队列研究新增7篇,使结论因果关联更具说服力。与该3项荟萃分析一样,本研究也证实短睡眠时间使MS患病风险增加,其内在机制可能与睡眠不足导致瘦素降低,生长素释放肽增加,从而产生饥饿感摄入更多热量导致肥胖[48],而肥胖除了是MS的组分外,也可以降低胰岛素的敏感性,与糖尿病的发生相关。此外,也有研究认为是下丘脑-垂体-肾上腺机制激活对睡眠和糖代谢产生影响[49]。本研究中,所有模型中均观察到短睡眠时间与MS均存在关联,队列的风险值(RR=1.13,95%CI:1.08~1.18)略大于横断面研究(OR=1.10,95%CI:1.04~1.16),但Ju和Choi[45]的研究中未发现短睡眠时间与MS相关(RR=1.62,95%CI:0.74~3.55),可能是由于相关文献数及样本量较少。
在总合并效应中,本研究显示长睡眠时间增加了MS患病风险(OR=1.10,95%CI:1.03~1.18)。Ju和Choi [45]在横断面设计中得到该结论(OR=1.23,95%CI:1.02~1.49),但在队列中并未观察到相同结果。本研究在研究设计的分组中均未发现长睡眠时间与MS的关联。这与Iftikhar等[47]和Xi等[46]的结论一致,二者纳入研究主要为横断面,风险值分别为1.13(95%CI:0.97~1.32)和1.07(95%CI:0.87~1.32)。亚组中未发现关联可能是由于样本量相对较少,合并后样本量增大,才使亚组中微弱的关联得以显示。长睡眠时间意味着体育锻炼时间减少、卧床时间增加,这对于脂肪代谢会产生影响,在一定程度上可以解释长睡眠时间与MS的正相关性。
亚组分析中,不同的种族、性别、年龄组及测量睡眠时段与MS的关联不同。<60岁人群睡眠时间过长或过短都会增加MS患病风险,这一关联在老年人中并不明显,可能由于老年人慢性病发病率较高,需要长期服药,药物对睡眠会存在潜在影响,而且慢性病与MS相关,但由于所能提取的信息有限,无法获得慢性病分组结果,故还需进一步研究证实。有趣的是,本研究发现睡眠时间与MS的关联在性别分布上相反,男性短睡眠时间与MS正相关,而女性长睡眠时间与MS正相关。女性睡眠时间过长可能会导致超重肥胖的发生率增高,而女性超重肥胖多为腹型肥胖,产生的健康问题要比男性更大,如高血压和心血管疾病[50],并且胰岛素抵抗与内脏肥胖密切相关。但由于亚组的研究数目不同,故应谨慎解释结果。
本研究存在局限性。首先,睡眠的测量方法大多为自我报告,导致得到的睡眠时间主观性较大;其次,MS定义并不一致,主要表现在组成成分及腹部肥胖的定义上,这可能使结果存在较大异质性;第三,短睡眠时间进行漏斗图Egger’s检验存在发表偏倚,但Begg’s检验并未得出相同结论,有待更多文献进行佐证;第四,由于信息的有限性,一些混杂因素不能充分考虑,如是否使用药物治疗或睡眠质量,因此对于结论需谨慎解释。
综上所述,本研究结果显示MS与长睡眠时间和短睡眠时间之间均存在关联。睡眠是一种可以改变的行为习惯,因此通过干预睡眠以降低MS患病风险具有重要的公共卫生意义。
利益冲突 所有作者均声明不存在利益冲突
致谢 感谢刘振(河北省人民医院办公室)对数据统计分析提供的宝贵意见
| [1] |
Alberti KGMM, Eckel RH, Grundy SM, et al. Harmonizing the metabolic syndrome:a joint interim statement of the international diabetes federation task force on epidemiology and prevention; national heart, lung, and blood institute; american heart association; world heart federation; international atherosclerosis society; and international association for the study of obesity[J]. Circulation, 2009, 120(16): 1640-1645. DOI:10.1161/CIRCULATIONAHA.109.192644 |
| [2] |
O'Neill S, O'Driscoll L. Metabolic syndrome:a closer look at the growing epidemic and its associated pathologies[J]. Obes Rev, 2015, 16(1): 1-12. DOI:10.1111/obr.12229 |
| [3] |
Deng HB, Tam T, Zee BCY, et al. Short sleep duration increases metabolic impact in healthy adults:A population-based cohort study[J]. Sleep, 2017, 40(10): zsx130. DOI:10.1093/sleep/zsx130 |
| [4] |
Song QF, Liu XX, Zhou WH, et al. Changes in sleep duration and risk of metabolic syndrome:the Kailuan prospective study[J]. Sci Rep, 2016, 6: 36861. DOI:10.1038/srep36861 |
| [5] |
Yoon HS, Lee KM, Yang JJ, et al. Associations of sleep duration with metabolic syndrome and its components in adult Koreans:from the health examinees study[J]. Sleep Biol Rhyth, 2016, 14(4): 361-368. DOI:10.1007/s41105-016-0065-7 |
| [6] |
Hamling J, Lee P, Weitkunat R, et al. Facilitating Meta-analyses by deriving relative effect and precision estimates for alternative comparisons from a set of estimates presented by exposure level or disease category[J]. Stat Med, 2008, 27(7): 954-970. DOI:10.1002/sim.3013 |
| [7] |
Hall MH, Muldoon MF, Jennings JR, et al. Self-reported sleep duration is associated with the metabolic syndrome in midlife adults[J]. Sleep, 2008, 31(5): 635-643. DOI:10.1093/sleep/31.5.635 |
| [8] |
Choi KM, Lee JS, Park HS, et al. Relationship between sleep duration and the metabolic syndrome:Korean national health and nutrition survey 2001[J]. Int J Obesity, 2008, 32(7): 1091-1097. DOI:10.1038/ijo.2008.62 |
| [9] |
左惠娟, 姚崇华, 胡以松, 等. 中国18~45岁男性人群行为习惯与代谢综合征的关系[J]. 中华流行病学杂志, 2011, 32(3): 235-238. Zuo HJ, Yao CH, Hu YS, et al. Relations between smoking, alcohol intake, physical activity, sleeping hours and the metabolic syndrome in Chinese male aged 18-45 years old[J]. Chin J Epidemiol, 2011, 32(3): 235-238. DOI:10.3760/cma.j.issn.0254-6450.2011.03.007 |
| [10] |
Najafian J, Toghianifar N, Mohammadifard N, et al. Association between sleep duration and metabolic syndrome in a population-based study:Isfahan healthy heart program[J]. J Res Med Sci, 2011, 16(6): 801-806. |
| [11] |
Kobayashi D, Takahashi O, Deshpande GA, et al. Relation between metabolic syndrome and sleep duration in Japan:A large scale cross-sectional study[J]. Int Med, 2011, 50(2): 103-107. DOI:10.2169/internalmedicine.50.4317 |
| [12] |
Choi JK, Kim MY, Kim JK, et al. Association between short sleep duration and high incidence of metabolic syndrome in midlife women[J]. Tohoku J Exp Med, 2011, 225(3): 187-193. DOI:10.1620/tjem.225.187 |
| [13] |
Arora T, Jiang CQ, Thomas GN, et al. Self-reported long total sleep duration is associated with metabolic syndrome:the Guangzhou biobank cohort study[J]. Diabetes Care, 2011, 34(10): 2317-2319. DOI:10.2337/dc11-0647 |
| [14] |
Wu MC, Yang YC, Wu JS, et al. Short sleep duration associated with a higher prevalence of metabolic syndrome in an apparently healthy population[J]. Prev Med, 2012, 55(4): 305-309. DOI:10.1016/j.ypmed.2012.07.013 |
| [15] |
McCanlies EC, Slaven JE, Smith LM, et al. Metabolic syndrome and sleep duration in police officers[J]. Work, 2012, 43(2): 133-139. DOI:10.3233/WOR-2012-1399 |
| [16] |
Sabanayagam C, Zhang RX, Shankar A. Markers of sleep-disordered breathing and metabolic syndrome in a multiethnic sample of US adults:results from the national health and nutrition examination survey 2005-2008[J]. Cardiol Res Pract, 2012, 2012: 630802. DOI:10.1155/2012/630802 |
| [17] |
Yoo H, Franke WD. Sleep habits, mental health, and the metabolic syndrome in law enforcement officers[J]. J Occupat Environ Med, 2013, 55(1): 99-103. DOI:10.1097/JOM.0b013e31826e294c3 |
| [18] |
Stefani KM, Kim HC, Kim J, et al. The influence of sex and age on the relationship between sleep duration and metabolic syndrome in Korean adults[J]. Diabetes Res Clin Pract, 2013, 102(3): 250-259. DOI:10.1016/j.diabres.2013.10.003 |
| [19] |
Lee J, Choi YS, Jeong YJ, et al. Poor-quality sleep is associated with metabolic syndrome in Korean adults[J]. Tohoku J Exp Med, 2013, 231(4): 281-291. DOI:10.1620/tjem.231.281 |
| [20] |
Chaput JP, McNeil J, Després JP, et al. Seven to eight hours of sleep a night is associated with a lower prevalence of the metabolic syndrome and reduced overall cardiometabolic risk in adults[J]. PLoS One, 2013, 8(9): e72832. DOI:10.1371/journal.pone.0072832 |
| [21] |
Hung HC, Yang YC, Ou HY, et al. The association between self-reported sleep quality and overweight in a Chinese population[J]. Obesity (Silver Spring), 2013, 21(3): 486-492. DOI:10.1002/oby.20259 |
| [22] |
Chaput JP, Mcneil J, Després JP, et al. Short sleep duration as a risk factor for the development of the metabolic syndrome in adults[J]. Prev Med, 2013, 57(6): 872-877. DOI:10.1016/j.ypmed.2013.09.022 |
| [23] |
Yu SS, Guo XF, Yang HM, et al. An update on the prevalence of metabolic syndrome and its associated factors in rural northeast China[J]. BMC Public Health, 2014, 14: 877. DOI:10.1186/1471-2458-14-877 |
| [24] |
Ohkuma T, Fujii H, Iwase M, et al. U-shaped association of sleep duration with metabolic syndrome and insulin resistance in patients with type 2 diabetes:the fukuoka diabetes registry[J]. Metabolism, 2014, 63(4): 484-491. DOI:10.1016/j.metabol.2013.12.001 |
| [25] |
Okubo N, Matsuzaka M, Takahashi I, et al. Relationship between self-reported sleep quality and metabolic syndrome in general population[J]. BMC Public Health, 2014, 14: 562. DOI:10.1186/1471-2458-14-562 |
| [26] |
Saleh D, Janssen I. Interrelationships among sedentary time, sleep duration, and the metabolic syndrome in adults[J]. BMC Public Health, 2014, 14: 666. DOI:10.1186/1471-2458-14-666 |
| [27] |
Wu J, Xu GQ, Shen LJ, et al. Daily sleep duration and risk of metabolic syndrome among middle-aged and older Chinese adults:cross-sectional evidence from the Dongfeng-Tongji cohort study[J]. BMC Public Health, 2015, 15: 178. DOI:10.1186/s12889-015-1521-z |
| [28] |
Li X, Lin LQ, Lv L, et al. U-shaped relationships between sleep duration and metabolic syndrome and metabolic syndrome components in males:A prospective cohort study[J]. Sleep Med, 2015, 16(8): 949-954. DOI:10.1016/j.sleep.2015.03.024 |
| [29] |
Kim JY, Yadav D, Ahn SV, et al. A prospective study of total sleep duration and incident metabolic syndrome:The ARIRANG study[J]. Sleep Med, 2015, 16(12): 1511-1515. DOI:10.1016/j.sleep.2015.06.024 |
| [30] |
Chang JH, Huang PT, Lin YK, et al. Association between sleep duration and sleep quality, and metabolic syndrome in Taiwanese police officers[J]. Int J Occupat Med Environ Health, 2015, 28(6): 1011-1023. DOI:10.13075/ijomeh.1896.00359 |
| [31] |
Yang LL, Xu ZG, He MA, et al. Sleep duration and midday napping with 5-year incidence and reversion of metabolic syndrome in middle-aged and older Chinese[J]. Sleep, 2016, 39(11): 1911-1918. DOI:10.5665/sleep.6214 |
| [32] |
Min H, Um YJ, Jang BS, et al. Association between sleep duration and measurable cardiometabolic risk factors in healthy korean women:the fourth and fifth korean national health and nutrition examination surveys (KNHANES Ⅳ and Ⅴ)[J]. Int J Endocrinol, 2016, 2016: 3784210. DOI:10.1155/2016/3784210 |
| [33] |
Lin SC, Sun CA, You SL, et al. The link of self-reported insomnia symptoms and sleep duration with metabolic syndrome:A Chinese population-based study[J]. Sleep, 2016, 39(6): 1261-1266. DOI:10.5665/sleep.5848 |
| [34] |
Suliga E, Kozieł D, Cieśla E, et al. Sleep duration and the risk of metabolic syndrome-A cross-sectional study[J]. Med Stud Stud Medy, 2017, 33(3): 169-175. DOI:10.5114/ms.2017.70342 |
| [35] |
Cole HV, Owusu-Dabo E, Iwelunmor J, et al. Sleep duration is associated with increased risk for cardiovascular outcomes:a pilot study in a sample of community dwelling adults in Ghana[J]. Sleep Med, 2017, 34: 118-125. DOI:10.1016/j.sleep.2017.03.008 |
| [36] |
Itani O, Kaneita Y, Tokiya M, et al. Short sleep duration, shift work, and actual days taken off work are predictive life-style risk factors for new-onset metabolic syndrome:a seven-year cohort study of 40000 male workers[J]. Sleep Med, 2017, 39: 87-94. DOI:10.1016/j.sleep.2017.07.027 |
| [37] |
van der Pal KC, Koopman ADM, Lakerveld J, et al. The association between multiple sleep-related characteristics and the metabolic syndrome in the general population:the New Hoorn study[J]. Sleep Med, 2018, 52: 51-57. DOI:10.1016/j.sleep.2018.07.022 |
| [38] |
Titova OE, Lindberg E, Elmståhl S, et al. Associations between the prevalence of metabolic syndrome and sleep parameters vary by age[J]. Front Endocrinol (Lausanne), 2018, 9: 234. DOI:10.3389/fendo.2018.00234 |
| [39] |
Kim CE, Shin S, Lee HW, et al. Association between sleep duration and metabolic syndrome:a cross-sectional study[J]. BMC Public Health, 2018, 18: 720. DOI:10.1186/s12889-018-5557-8 |
| [40] |
周娟, 曾志伟, 王长义, 等. 睡眠总时长与代谢综合征的相关性研究[J]. 中国慢性病预防与控制, 2019, 27(1): 1-5. Zhou J, Zeng ZW, Wang CY, et al. The correlation between total sleep duration and metabolic syndrome[J]. Chin J Prev Contr Chron Dis, 2019, 27(1): 1-5. DOI:10.16386/j.cjpccd.issn.1004-6194.2019.01.001 |
| [41] |
陈梦雪, 李丹婷, 张啸, 等. 成都市成年人夜间睡眠时长、午间睡眠时长与代谢综合征的关系[J]. 现代预防医学, 2019, 46(8): 1439-1442,1467. Chen MX, Li DT, Zhang X, et al. Association between nocturnal sleep duration and daytime napping with metabolic syndrome among adults in Chengdu[J]. Mod Prev Med, 2019, 46(8): 1439-1442,1467. |
| [42] |
张爽, 李莲, 黄育北, 等. 成年人睡眠时间对体重增加和肥胖风险的Meta分析[J]. 中华流行病学杂志, 2015, 36(5): 519-525. Zhang S, Li L, Huang YB, et al. Meta-analysis of prospective cohort studies about sleep duration and risk of weight gain and obesity in adults[J]. Chin J Epidemiol, 2015, 36(5): 519-525. DOI:10.3760/cma.j.issn.0254-6450.2015.05.023 |
| [43] |
张永军. 睡眠时间与高血压相关性的Meta分析[J]. 中国动脉硬化杂志, 2019, 27(6): 522-527. Zhang YJ. Meta-analysis of the relationship between sleep duration and hypertension[J]. Chin J Arterioscler, 2019, 27(6): 522-527. DOI:10.3969/j.issn.1007-3949.2019.06.012 |
| [44] |
朱婧菡, 吕梦莲, 尹洁云, 等. 睡眠时间与妊娠期糖尿病发病风险关系的Meta分析[J]. 现代预防医学, 2019, 46(10): 1729-1732,1747. Zhu JH, Lv ML, Yin JY, et al. Sleep duration and risk of gestational diabetes mellitus:a Meta-analysis of cohort study[J]. Mod Prev Med, 2019, 46(10): 1729-1732,1747. |
| [45] |
Ju SY, Choi WS. Sleep duration and metabolic syndrome in adult populations:a Meta-analysis of observational studies[J]. Nutr Diabetes, 2013, 3: e65. DOI:10.1038/nutd.2013.8 |
| [46] |
Xi B, He D, Zhang M, et al. Short sleep duration predicts risk of metabolic syndrome:a systematic review and Meta-analysis[J]. Sleep Med Rev, 2014, 18(4): 293-297. DOI:10.1016/j.smrv.2013.06.001 |
| [47] |
Iftikhar IH, Donley MA, Mindel J, et al. Sleep duration and metabolic syndrome. An updated dose-risk Meta-analysis[J]. Ann Am Thorac Soc, 2015, 12(9): 1364-1372. DOI:10.1513/AnnalsATS.201504-190OC |
| [48] |
Taheri S, Lin L, Austin D, et al. Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index[J]. PLoS Med, 2004, 1(3): e62. DOI:10.1371/journal.pmed.0010062 |
| [49] |
Vgontzas AN, Liao DP, Pejovic S, et al. Insomnia with short sleep duration and mortality:the Penn State cohort[J]. Sleep, 2010, 33(9): 1159-1164. DOI:10.1093/sleep/33.9.1159 |
| [50] |
Tan X, Chapman CD, Cedernaes J, et al. Association between long sleep duration and increased risk of obesity and type 2 diabetes:A review of possible mechanisms[J]. Sleep Med Rev, 2018, 40: 127-134. DOI:10.1016/j.smrv.2017.11.001 |
 2020, Vol. 41
2020, Vol. 41