b Department of Physics and Tianjin Key Laboratory of Low Dimensional Materials Physics and Preparing Technology, School of Science, Tianjin University, Tianjin 300350, China
Radiotherapy had been widely used in the process of cancer treatment, but its side effects limited its wider application to some extent [1-6]. Ultrahigh radiation doses during the radiotherapy can cause great acute or irreversible damages to those healthy tissues and organs near the tumor lesion, which usually causes many undesirable complications. Lots of reactive oxygen species (ROS) will be largely generated as a result of water radiolysis. These radicals can quickly react with nearby molecules, resulting in chemical bonds break off and biomolecules oxidation (addition of oxygen atoms), such as DNA, lipids and proteins [7-11], which will consequently cause cellular and tissue damages [12-14]. Thereby, it is an urgent need to develop high-efficient radioprotectants for protecting healthy tissues with minimum adverse effects.
Due to their unique physical and chemical properties, catalytic nanomaterials have been used in different fields such as photodetectors [15, 16], optical sensors [17-21], field-effect transistors [22-24] and biomedicine [25-34]. A class of Platinum (Pt) or Ptbased nanomaterials had been produced and showed high catalytic properties for decomposing H2O2 via improving oxygen reduction reactions. Pt nanomaterials, with different sizes or structures, had been utilized in biomedical field for their outstanding free radicals' killing ability [35-39]. Recently, several groups have discovered that Palladium (Pd) also displayed apparent antioxidant catalytic activity [40-43]. It had been demonstrated that the bimetal nanocrystals exhibit high catalytic activities with high-index facets [44, 45]. Thus, it is interesting to explore the radiation protection effects with bimetal nanocrystals for decreasing side effects.
In this work, we devised and synthesized PtPd hollow nanocubes by one-pot synthesis method [46]. The PtPd hollow nanocubes in our work are a new type of zero-dimensional nanomaterial with high-index facets, which can bring larger specific surface area and will provide more surface active sites per unit mass. Moreover, its high-index facet structure causes its rougher surface. In this kind of nanocubes, there will be more dangling keys, which will largely improve its catalytic activity. Thereby, we considered that this kind of nanocubes deserved to be used for radiation protection. To explore their radioprotection properties, we designed a series of biological experiment protocols in vitro and in vivo. It was found that PtPd nanocubes could obviously increase the cell survival rate and decrease the intracellular ROS level after 4 Gy radiation. In vivo experiments showed that the survival rate of mice was about 40% after 7.2 Gy radiation, suggesting the apparent radioprotection effect of the asprepared PtPd nanocubes. PtPd nanocubes can served as an effective free radical scavenger by decreasing oxidative DNA damage and MDA level and increasing SOD activities in mice.
Our preparations and experimental protocols include following materials: Palladium acetylacetonate (Pd(acac)2, 99%) and platium acetylacetonate (Pt(acac)2, 98%) were purchased from Shanghai Macklin Biochemical Co., Ltd. (China). PVP (MW=30000, AR), and dimethyl formamide (DMF, AR) and sodium iodide (NaI, AR) were purchased from Shanghai Aladdin Biochemical Co., Ltd (China). Ultrapure water (Millipore, 18.2 MΩ cm) was used in whole experiments and all reagents in our experiments were not further purified before using.
Synthesis of hollow PtPd nanocube: Pt(acac)2 (30 mg), Pd(acac)2 (25 mg), PVP (160 mg) and DMF (10 mL) were added into an NaI solution (2 mL, 0.15 mg/mL) and mixed together. Such uniform solution were heated at 150 ℃ for 8 h after transferring into a Teflon-lined stainless-steel autoclave. Then, the solution were cooled down to room temperature, and acetone and ethanol were added to obtain the precipitated products, respectively. Removed excess reactants and centrifugated at 12, 000 rpm for 10 min. The precipitate was purified with PBS (pH 7.4) with several centrifugation. Finally, the as-prepared hollow PtPd nanocubes were dissolved in PBS for following characterization and biological investigation.
Characterization of hollow PtPd nanocubes: TEM and HRTEM images of the prepared PtPd sample were performed on JEM-2100F (JEOL, Japan) that operated at 200 kV. XRD pattern was performed by D8 Advance (Bruker, Germany) with the Cu Kα radiation. Hydrodynamic diameter of the hollow PtPd nanocubes were measured by Malvern Zetasizer Nano ZS90.
Catalytic activities for H2O2 reduction: CV measurements were conducted on an electrochemical analyzer (CHI660D, Shanghai) to evaluate the catalytic activities for H2O2 reduction, which were set at a scan rate of 50 mV/s. There are three electrode cells: counter electrode and reference electrode were platinum wire and saturated calomel electrode respectively, while the working electrode was prepared by dropping PtPd solution (0.5 mg/mL) on a glassy-carbon electrode and drying at the atmospheric pressure. Upon adding 3 mL Nafion solution on the working electrode, the measurements will be operated.
Total antioxidant capacity assay in vitro: According to a rapid ABTS method, the total antioxidant capacity of PtPd nanocubes were detected under an ultraviolet spectrophotometer (UV3600, Shimadzu, Japan). The detailed process was as follow: ABTS working solution preparation (160 μL detection buffer, 10 μL ABTS solution and 10 μL H2O2 solution after diluting 1000 times), 20 μL of the as-prepared PtPd solution with different concentration were added into working solution above for 1 h, and the mixture was incubated at room temperature. The mixture was then centrifuged at 12, 000 rpm for 10 min, and the absorbance was measured at 414 nm and 734 nm separately.
Cellular toxicity assay in vitro: The high glucose Dulbecco's modified Eagle medium (DMEM) supplemented with 10% FBS (Gibco), penicillin (100 units/mL) and streptomycin (100 mg/mL) were used in all cellular experiments. The Chinese Hamster Ovary (CHO) cells were inoculated into 96-well plates (about 4500 cells per well) and cultured at an environment of 37 ℃, 5% CO2 and suitable humidity for 24 h. Replace the original DMEM with different concentrations (0, 0.41, 1.23, 3.7, 11, 33, 100, 300 μg/mL) of hollow PtPd solution that dissolved in fresh DMEM, and the cells were continued to incubated for 24 h and 48 h. Cytotoxicity of as-prepared PtPd nanocubes was determined by MTT assay.
Intracellular radiation protection: The radiation equipment were provided by the Institute of Radiation Medicine, Chinese Academy of Medical Sciences. CHO cells (about 4500 per well) were seeded into 96-well plates. Before 30 min radiation, all cells were treated with new DMEM containing PtPd nanocubes at the concentration of 0, 0.4, 1.2 and 3.6 μg/mL. After 4 Gy γ-radiation, CHO cells were kept for another 24 h. Cell survival rate was tested by MTT assay as well.
Relative ROS level in vitro: CHO cells were planted into 6-well plates (about 105 per well) and cultured for 24 h. The PtPd nanocube solution at a concentration of 3.6 μg/mL were added into each well and cultured for 30 min before 4 Gy radiation. The plates were continually kept for another 24 h. The DCFH-DA agent was added into each well and incubated for 20 min to load such probe. After washing by PBS three times, the qualitative image results were collected through a fluorescent microscope (AMG, EVOS), and the quantitative relative ROS results were gathered and analyzed by flow cytometer (BD).
In vivo radiation protection: All the male C57BL/6 mice used in our experiment were purchased and treated according to the requirements of the Institutional Animal Care and Use Committee (IACUC) and the Institute of Radiation Medicine, Chinese Academy of Medical Sciences. Mice were divided into two groups (n = 10) randomly, including radiation only group and radiation with PtPd treated group. All mice were raised at SPF level environment under 12 h dark/light circles, with free feeding. Each group was intraperitoneally injected with 200 μL the saline solution and the as-prepared sample (5 mg/mL) respectively, and then recieved the 7.2 Gy gamma rays (137Cs, 3600 Ci). The mice survival rates of 30 days were monitored every two days.
Analysis of BMNC and bone marrow DNA: Thirty mice were assigned into 6 groups (n =5), namely the radiation only group for 1 day and 7 days, the control group for 1 day and 7 days, the radiation with PtPd treated group for 1 day and 7 days. The controls (without radiation) and radiation only group were injected with the saline solution, while the rest group were treated as-prepared sample solution intraperitoneally (5 mg/mL), and then received 7 Gy radiation. After 1 day and 7 days, all mice were sacrificed and both sides of their femurs were collected respectively. To assess the amount of DNA from bone marrow, the femur without other connective tissue was flushed by 0.005 mol/L calcium chloride solution, and as-prepared sample was been saved at 4 ℃ for 2 h. After being centrifuged at 2500 rpm for 15 min, the precipitate was collected up and mixed with 0.2 mol/L perchloric acid. And this mixture was kept in boiling water bath for another 15 min. Sample at room temperature was filtered and determined under 268 nm by UV–vis spectrophotometer (Shimadzu, UV-1750). To evaluate the level of BMNC, the femur without other connective tissue was flushed by PBS to obtain the bone marrow cell suspension; the suspension was filtrated and counted by the blood cell counting instrument (Mindray, BC-2800Vet).
Analysis of SOD and MDA level: After scarifying mice above at the 1st and the 7th day respectively, the organs of liver and lung of each group were gathered and homogenized in saline solution (m: v= 1:9). According to the instruction manual of both testing kits (Beyotime, S0109 and S0131), SOD and MDA level of samples were detected under 560 nm or 532 nm using UV–vis spectrophotome-ter (Shimadzu, UV-1750).
Assessment of hematology and biochemistry: Twenty-four C57BL/6 mice were divided into 3 groups, the radiation only group, the radiation with PtPd treated group and the control group (8 mice in each group). The control (without radiation) and radiation only group were injected with the saline solution, while the rest group were treated as-prepared sample solution intraperitoneally (5 mg/mL), and received 7 Gy radiation. After 30 days' treatment, all mice were executed and the blood cells were collected. The haematological parameters were measured by the blood cell counting instrument (Mindray, BC-2800Vet). Other parts of the blood samples were centrifuged at 4500 rpm for 10 min to gather serum, and then these serum samples were detected under special analyzer (HITACHI 7180) to obtain biochemistry parameters.
Statistical analysis: All of the data were expressed as average ± standard deviations (SD). Analysis of variance (ANOVA) statistics were performed, and P-values less than 5% were considered to be statistically significant.
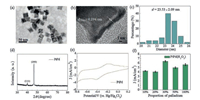
PtPd nanocubes were synthesized through a simplified one-pot method. As shown in Figs. 1a and c, the average size of PtPd nanocubes is 23.53 ± 2.09 nm. The high-resolution transmission electron microscopy (HRTEM) image shown in Fig. 1b displayed that there were unique concaves in PtPd nanocubes, suggesting forming the hollow structure. Meanwhile, HRTEM image also demonstrated that the lattice spacing of single nanocube is about 0.194 nm. Fig. 1d further confirmed the cubic structure of the assynthesized PtPd nanocubes by X-ray diffraction. To confirm the catalytic activities of the nanocubes in H2O2 reduction, the cyclic voltammetry measurements were conducted at a scan rate of 50 mV/s. As shown in Figs. 1e and f, different proportions of PtPd component (10%, 20%, 30%, 50% and 100%) have different H2O2 catalytic capability. The high current density represents high ability of H2O2 reduction. According to the results, it is clear that PtPd nanocubes of 30% proportion exhibit the best catalytic activities.
|
Download:
|
| Fig. 1. Characterization of PtPd nanocubes: (a) TEM image, (b) HRTEM image, (c) Size distribution, (d) XRD pattern and (e) CVs of GC electrode of PtPd nanocubes. (f) Corresponding catalytic activities at different proportion of Pd element in PtPd complex nanocrystals. | |
The properties of most nanocrystals are strongly connected with their size, shape, and surface structure. Recently, the fabrication of nanoparticles enclosed by high-index facets is becoming a hotspot in nano-research area. Generally speaking, the high density of low-coordinated atoms in the forms of atomic steps and kinks, high-index facets, are easy to be more active toward specific reactions than low-index planes which are composed of closely packed surface atoms [47]. In this work, we also studied the difference between the two kinds of PtPd nanocubes with highindex or low-index facets. The total antioxidant activity of PtPd nanocubes were measured with the ABTS assay kits. With the interaction between ABTS and oxidant, ABTS solution will be converted into a green ABTS·+ solution, while the production of ABTS·+ can be inhibited in the presence of antioxidants. By measuring the absorbance of ABTS·+ at 414 nm or 734 nm, we can indirectly calculate out the total antioxidant activity of PtPd samples. In Fig. 2a, we found that both the absorbance of PtPd nanocubes with high-index facets at 414 nm and 734 nm were increased with elevated concentrations, and the absorbance at 414nm was higher than the one at 734 nm. In Fig. 2b, by selecting 734 nm as the measurement wavelength, and 0.1 mg/mL as the measurement concentration, we found that the absorbance had a continuous increase in the first 750 min and the changes of absorbance value were becoming gentle gradually thereafter. These results revealed that our PtPd nanocubes with high-index facets had obvious antioxidant capacities, and such activities could last for 10 min at least. We also performed the same series of tests on the PtPd nanocubes with low-index facets samples. The results were displayed in Supporting information. We can notice that the highest absorbance value of PtPd nanocubes with low-index facets at 414 nm and 734 nm are 1.3 and 0.7, respectively, which are evidently lower than the PtPd nanocubes with high-index facets (Fig. S1a in Suporting information). Besides, we can see from Fig. S1b (Supporting information) that the relative total absorbance of low-index group is only about 1/6 of high-index group, although the trend of absorbance value change seemed to be no differences. Based on these evidences above, we considered that the asprepared PtPd nanocubes with high-index facets have better antioxidant activities than the low-index facets ones. In order to further explore the stability of PtPd nanocubes with high or lowindex facets, we detected the absorbance of the same samples at the first time and a week later. As shown in Figs. 2c and d, the value nearly had no obvious changes, which indicated that as-prepared PtPd nanocubes show high stability. In this part, we cleared that the crystal facet will influence the catalytic properties of PtPd nanocubes, and the high-index facets will exhibit more active antioxidant effects than the low-index facets. To explore the biological activities of the PtPd nanocubes with high-index facets on cells or mice, we carried on the biological experiments in the next parts.

|
Download:
|
| Fig. 2. Antioxidant capacities of PtPd nanocubes: (a) UV absorbance of PtPd nanocubes with high-index facets in different concentrations (0, 0.2, 0.4, 0.6, 0.8, 1 mg/mL) at 414 nm and 734 nm. (b) Time dependent absorbance of 0.1 mg/mL PtPd nanocubes with high-index facets at 734 nm. (c, d) 414 nm UV absorbance of 0.1 mg/mL PdPd nanocubes with high or low-index facets in a week. | |
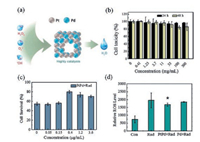
To assess the cytotoxicity and radiation protection in vitro, the MTT (3-(4, 5)-dimethylthiahiazo 3, 5-di-phenytetrazoliumromide) assays were conducted by calculating the survival rate of CHO cells. As shown in Fig. 3b, it is clearly demonstrated that PtPd nanocubes almost caused no cytotoxicity to CHO cells even at the dose up to 300 μg/mL after 24- or 48-h incubation. Before 4 Gy radiation, CHO cells were treated with different concentrations of PtPd nanocubes (0, 0.4, 1.2, 3.6 μg/mL). Fig. 3c shows that PtPd treated groups have apparent higher survival rate compared with radiation only group. Among these, cell survival rate of 0.4 μg/mL group was almost recovered up to 80%, which indicated the in vitro radiation protection of PtPd nanocubes. To further discuss the protective principle in vitro, quantitative analysis of intracellular ROS level was conducted by a flow cytometer. Fig. 3d shows that after radiation at a dose of 4 Gy, intracellular ROS level rose sharply by 2.7 times compared with control group, while the amount of increase was reduced to 2.3 times with administration of PtPd nanocubes. Comparing with the 100% Pd treated group, ROS level of PtPd-treated group decreased about 12%. According to all in vitro results above, we confirmed that PtPd nanocubes show high free radicals scavenging activities. The biological toxicity of Pt or Ptbased nanomaterials have been reported in many studies [48, 49]. However, the PtPd nanocubes in our study are different in size and shape compared with their nanomaterials. For biomedicine use, the nanomaterials always need toxicity evaluation. Compared with in vivo tests, cytotoxicity evaluation is more economical and faster. Shaw et al. found that in vitro assay could be a predictor of in vivo responses [50, 51].
|
Download:
|
| Fig. 3. Cytotoxicity and radioprotection in vitro of PtPd nanocubes: (a) The illustration of the structure of the PtPd nanocube and its catalysis effect on oxidative free radicals. (b) Cell toxicity of different concentrations of PtPd nanocubes (0, 0.41, 1.23, 3.7, 11, 33, 100, 300 μg/mL). (c) Cell survival rate of different concentrations of PtPd nanocubes (0, 0.4, 1.2, 3.6 μg/mL) after 4 Gy radiation. (d) Quantitative analysis of intracellular ROS level among the control, the radiation only, the PtPd treated group and the Pd treated group (* indicates P < 0.1 as compared with the radiation only group). | |
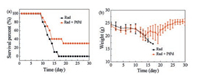
To test compounds or medical materials have radiation protection effects or not, the survival rate in 30 days of irradiated mice is always employed as a gold indicator. The results of 30 days survival rate were shown in Fig. 4a. Comparing to the radiation only group, we found that the as-prepared sample (200 μL/mouse, at a concentration of 5 mg/mL) not only prolonged mice survival time, but also improved mice survival rate after exposing to 7.2 Gy 137Cs radiation. To further verify the toxicity of PtPd nanocubes in vivo, we had noted down the weight changes of the irradiated mice with or without PtPd nanocubes treatment in 30 days. As indicated in Fig. 4b, there was only a slight weight decrease in the first 10 days, and it soon recovered to normal level later on. But the body weight of the untreated mice declined until all the mice died. In general, if the survival rate of administrated group is 30% higher than the control irradiated-only group, we can infer that the tested compound or material might have a potential for radioprotection [52]. Therefore, C57BL/6 mice were purchased and raised according to our previous experiments to explore the radioprotection of PtPd nanocubes in vivo. Thereby, the as-synthetic PtPd nanocubes can protect the mice from radiation damage. In addition, it seemed to have no apparent and non-reversible toxicity in vivo.
|
Download:
|
| Fig. 4. (a) The 30 days survival rate of mice with or without treatment of PtPd nanocubes after 7.2 Gy radiation. (b) Body weight changes of irradiated mice within 30 days with or without treatment of PtPd nanocubes. | |
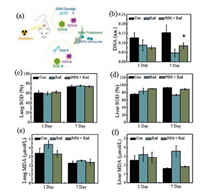
Based on the results of ROS test in vitro, it is clear that the PtPd nanocubes can effectively decrease cell ROS damages. To further discuss the mechanisms of in vivo radioprotection effects of PtPd nanocubes (Fig. 5a), we designed a series of experiments including the total DNA assay (one of the most sensitive and typical indicators of radiation damages), the SOD activity and MDA level measurement in mice. Fig. 5b demonstrated the changes of DNA in mice after radiation in one or seven days. It is clear that radiation lead to rapid decrease of total DNA amount, but after PtPd nanocubes treatment, the amount of total DNA in mice was increased by 2 times compared to radiation only group at the 7th day, which indicated that the PtPd nanocubes may have DNA protection effects. After initial radiation, changes on the amount and structures of DNA can directly reflect the extent of radiation damage and the degree of dose-sensitivity [53]. At the same dose of radiation, the more DNA damage, the higher sensitivity or radiation doses. Namely, if the amount of damaged DNA at the same dose was reduced by treating with the tested compounds or materials, it is reasonable to infer that they probably have radiation protection effects.
|
Download:
|
| Fig. 5. Radiation protection in vivo of PtPd nanocubes: (a) The sketch map of the PtPd nanocubes treatment influencing the DNA damage, SOD and MDA levels in irradiated mice. (b) Total DNA amount, * indicates P < 0.05 as compared with the control group. SOD activities in lung (d) and liver (d) of each group. MDA levels in lung (e) and liver (f) of each group. | |
As shown in Figs. 5c-f, that radiation caused the increase of free radicals in vivo and the level of SOD and MDA shows significant changes. No significant reduction was observed on SOD level after 1-day PtPd treatment, but SOD can partially recover after 7-day treatment (Figs. 5c and d). Figs. 5e and f displayed the change of MDA level in lung and liver respectively. As it shows, PtPd nanocubes can largely reduce MDA damages in vivo that induced by radiation at the 1th and 7th day. Superoxide dismutase (SOD) is an important natural antioxidant enzyme in scavenging free radicals, and its level indicates the aging or injury condition of organic bodies. More and more studies are focusing on radiation protection effects and the mechanisms of SOD and its analogues. Mn-SOD was reported to prevent the development of radiationinduced esophagitis and modulated cytokine expression, to decrease the extent of radiation-induced ulceration in patients receiving head and neck radiation [54-57]. Malondialdehyde (MDA) is an end product of lipid peroxidation by reacting with free radicals. That is to say, the more free radicals, the higher MDA levels. Those results suggest that PtPd nanocubes show good capability of free radicals scavenging, suggesting its activity mechanisms related to SOD analogues.
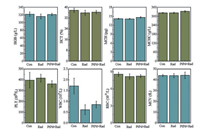
Finally, haematopoietic system is one of the most sensitive organs to radiation damages, and thus protection for hematopoietic system plays an important role in effect evaluation. As shown in Fig. 6, the haematology analysis was measured at 30 days. After radiation, the number of white cells (WBC), red cells (RBC) and haemoglobin (HGB) was decreased apparently compared with the control group, however, these indicators of the group treated with PtPd nanocubes recovered partially.
|
Download:
|
| Fig. 6. Hematological analysis of irradiated mice treated with or without PtPd nanocubes. | |
As we know, small molecule radioprotectants always show limited short blood circulation time, like Amifostine. It is a problem that needed to be solved for a long time. But nanomaterials with relatively large hydrodynamic size overcome this disadvantage and then give stable protection effect. As a kind of biomedical materials, PtPd bimetal nanocrystals, in this study, showed significant oxidative free radicals killing activities and prominent protection effect on irradiated mice. Although it can be expected for its protection use in cancer radiotherapy or other fields, more in-depth studies are needed to clear its pharmacokinetic or other properties in vivo, like biodistribution, renal clearance, etc.
In summary, we developed highly catalytic PtPd nanocubes and investigated its radiation protection effects in our paper. In vitro experiments indicated that PtPd nanocubes with high-index facets exhibited excellent catalytic activities and free radicals scavenging capabilities. In vivo experiment showed that 30% survival rate of mice can be achieved by PtPd nanocubes treatment, indicating its potential radioprotection activity. Other evidences like SOD activity improvement, MDA level reduction, total DNA recovery and hematopoietic system protection further reveal that the hollow PtPd nanocubes exhibit significant protection effect against high energy ray.
AcknowledgmentsThis work was supported by the National Natural Science Foundation of China (Nos. 81673106, 81471786 and 91859101) and CAMS Innovation Fund for Medical Science (No. 2017-12M-1012).
Appendix A. Supplementary dataSupplementary material related to this article can be found, in the online version, at doi:https://doi.org/10.1016/j.cclet.2019.03.044.
| [1] |
S. Tanguturi, B. Alexander, Neurol. Clin. 36 (2018) 599-625. DOI:10.1016/j.ncl.2018.04.012 |
| [2] |
A. Hong, D. Jones, R. Boyle, P. Stalley, Clin. Oncol. 30 (2018) 589-592. DOI:10.1016/j.clon.2018.05.002 |
| [3] |
M.A. Armanious, H. Mohammadi, S. Khodor, et al., Curr. Probl. Cancer 42 (2018) 433-442. DOI:10.1016/j.currproblcancer.2018.05.008 |
| [4] |
W. Haque, V. Verma, P. Polamraju, et al., Radiother. Oncol. 129 (2018) 264-269. DOI:10.1016/j.radonc.2018.07.008 |
| [5] |
J. Chang, S. Kim, Y. Kim, et al., Gynecol. Oncol. 151 (2018) 39-45. DOI:10.1016/j.ygyno.2018.08.012 |
| [6] |
F. De Felice, V. Tombolini, Crit. Rev. Oncol. Hematol. 128 (2018) 82-87. DOI:10.1016/j.critrevonc.2018.06.002 |
| [7] |
P.M.K.S. Shyama, A. D'Costa, S. Kadam, B. Sonaye, R. Chaubey, Ecotoxicol. Environ. Saf. 144 (2017) 166-170. DOI:10.1016/j.ecoenv.2017.06.022 |
| [8] |
J. Cadet, K.J.A. Davies, Free Radic. Biol. Med. 107 (2017) 2-12. DOI:10.1016/j.freeradbiomed.2017.03.030 |
| [9] |
M. Majidinia, B. Yousefi, DNA Repair (Amst.) 54 (2017) 22-29. DOI:10.1016/j.dnarep.2017.03.009 |
| [10] |
K.N. Mishra, B.A. Moftah, G.A. Alsbeih, Biomed. Pharmacother. 106 (2018) 610-617. DOI:10.1016/j.biopha.2018.06.150 |
| [11] |
H. Wang, X. Mu, H. He, X.D. Zhang, Trends Pharmacol. Sci. 39 (2018) 24-48. DOI:10.1016/j.tips.2017.11.003 |
| [12] |
G. Wang, S. Deng, J. Liu, et al., Ecotoxicol. Environ. Saf. 144 (2017) 315-320. DOI:10.1016/j.ecoenv.2017.06.024 |
| [13] |
J. Wang, T. Li, J. Feng, et al., Environ. Toxicol. Pharmacol. 60 (2018) 128-137. DOI:10.1016/j.etap.2018.04.014 |
| [14] |
M. Kamran, A. Ranjan, N. Kaur, S. Sur, V. Tandon, Med. Res. Rev. 36 (2016) 461-493. DOI:10.1002/med.21386 |
| [15] |
J. Chao, S. Xing, Y. Zhao, et al., Solid State Sci. 61 (2016) 51-57. DOI:10.1016/j.solidstatesciences.2016.09.002 |
| [16] |
J. Chao, S. Xing, Z. Liu, et al., Mater. Res. Bull. 98 (2018) 194-199. DOI:10.1016/j.materresbull.2017.10.026 |
| [17] |
N. Ullah, M. Mansha, I. Khan, A. Qurashi, Trends Analyt. Chem. 100 (2018) 155-166. DOI:10.1016/j.trac.2018.01.002 |
| [18] |
Y. Ding, S. Wang, J. Li, L. Chen, Trends Analyt. Chem. 82 (2016) 175-190. DOI:10.1016/j.trac.2016.05.015 |
| [19] |
G. Maduraiveeran, M. Sasidharan, V. Ganesan, Biosens. Bioelectron. 103 (2018) 113-129. DOI:10.1016/j.bios.2017.12.031 |
| [20] |
A. Zamora-Gálvez, E. Morales-Narváez, C.C. Mayorga-Martinez, A. Merkoçi, Appl. Mater. Today 9 (2017) 387-401. DOI:10.1016/j.apmt.2017.09.006 |
| [21] |
K. Ngamdee, T. Tuntulani, W. Ngeontae, Sensor. Actuat. B: Chem. 216 (2015) 150-158. DOI:10.1016/j.snb.2015.04.019 |
| [22] |
A. Nehra, K. Pal Singh, Biosens. Bioelectron. 74 (2015) 731-743. DOI:10.1016/j.bios.2015.07.030 |
| [23] |
T.T. Tran, A. Mulchandani, Trends Analyt. Chem. 79 (2016) 222-232. DOI:10.1016/j.trac.2015.12.002 |
| [24] |
C. Xiong, Y. Wang, H. Qu, et al., Sensor. Actuat. B: Chem. 246 (2017) 235-242. DOI:10.1016/j.snb.2017.02.025 |
| [25] |
C. Ramamurthy, M. Padma, I. Samadanam, et al., Colloids Surf. B: Biointerfaces 102 (2013) 808-815. DOI:10.1016/j.colsurfb.2012.09.025 |
| [26] |
X.D. Zhang, Z. Luo, J. Chen, et al., Small 11 (2015) 1683-1690. DOI:10.1002/smll.201402233 |
| [27] |
X.D. Zhang, J. Chen, J. Yang, et al., J. Mater. Chem. B 3 (2015) 4735-4741. DOI:10.1039/C5TB00411J |
| [28] |
S. Hernando, O. Gartziandia, E. Herran, et al., Nanomedical 11 (2016) 1267-1285. DOI:10.2217/nnm-2016-0019 |
| [29] |
C. He, X. Duan, N. Guo, et al., Nat. Commun. 7 (2016) 12499. DOI:10.1038/ncomms12499 |
| [30] |
X.D. Zhang, J. Chen, Y. Min, et al., Adv. Func. Mater. 24 (2014) 1718-1729. |
| [31] |
X. Mu, J.Y. Wang, X. Bai, et al., ACS Appl. Mater. Interfaces 9 (2017) 20399-20409. DOI:10.1021/acsami.7b02900 |
| [32] |
X. Bai, J. Wang, X. Mu, et al., ACS Biomater. Sci. Eng. 3 (2017) 460-470. DOI:10.1021/acsbiomaterials.6b00714 |
| [33] |
W. Long, J. Wang, J. Yang, et al., J. Biomed. Nanotechnol. 15 (2019) 62-76. DOI:10.1166/jbn.2019.2665 |
| [34] |
X.D. Zhang, J. Zhang, J. Wang, et al., ACS Nano 10 (2016) 4511-4519. DOI:10.1021/acsnano.6b00321 |
| [35] |
F. Xu, X. Mu, J. Wang, et al., J. Biomed. Nanotechnol. 13 (2017) 1512-1521. DOI:10.1166/jbn.2017.2468 |
| [36] |
M.D.C. Gimenez-Lopez, A. Kurtoglu, D.A. Walsh, A.N. Khlobystov, Adv. Mater. 28 (2016) 9103-9108. DOI:10.1002/adma.201602485 |
| [37] |
C. Goswami, K.K. Hazarika, P. Bharali, Mater. Sci. Energy Technol. 1 (2018) 117-128. |
| [38] |
J. Qu, H. Liu, F. Ye, W. Hu, J. Yang, Int. J. Hydrogen Energy 37 (2012) 13191-13199. DOI:10.1016/j.ijhydene.2012.03.122 |
| [39] |
H.M. Chen, R.S. Liu, M.Y. Lo, et al., J. Phys. Chem. C 112 (2008) 7522-7526. |
| [40] |
F.A. Gutierrez, I.S. Giordana, V.C. Fuertes, et al., Microchem. J. 141 (2018) 240-246. DOI:10.1016/j.microc.2018.05.019 |
| [41] |
M. Islam, P. Mondal, A.S. Roy, K. Tuhina, J. Mater. Sci. 45 (2010) 2484-2493. DOI:10.1007/s10853-010-4220-2 |
| [42] |
J. Gegner, G. Hörz, R. Kirchheim, J. Mater. Sci. 44 (2008) 2198-2205. |
| [43] |
J. Liu, H. Zhou, Q. Wang, F. Zeng, Y. Kuang, J. Mater. Sci. 47 (2011) 2188-2194. |
| [44] |
Y. Zhang, L. Zhao, J. Walton, Z. Liu, Z. Tang, Int. J. Hydrogen Energy 42 (2017) 17112-17121. DOI:10.1016/j.ijhydene.2017.05.167 |
| [45] |
J.Y. Wang, X. Mu, Y. Li, et al., Small 14 (2018) e1703736. DOI:10.1002/smll.201703736 |
| [46] |
X. Huang, H. Zhang, C. Guo, Z. Zhou, N. Zheng, Angew. Chem. Int. Ed. 48 (2009) 4808-4812. DOI:10.1002/anie.200900199 |
| [47] |
X. Huang, Z. Zhao, J. Fan, Y. Tan, N. Zheng, J. Am. Chem. Soc. 133 (2011) 4718-4721. DOI:10.1021/ja1117528 |
| [48] |
P.V. Asharani, Y.L. Wu, Z.Y. Gong, S. Valiyaveettil, Nanotoxicology 5 (2011) 43-54. DOI:10.3109/17435390.2010.489207 |
| [49] |
A. Elder, H. Yang, R. Gwiazda, et al., Adv. Mater. 19 (2007) 3124-3129. DOI:10.1002/adma.200701962 |
| [50] |
K. Bhattacharya, G. Kilic, P.M. Costa, B. Fadeel, Nanotoxicology 11 (2017) 809-826. |
| [51] |
J. Gopal, N. Hasan, M. Manikanda, H.F. Wu, Sci. Rep. 3 (2013) 1260. DOI:10.1038/srep01260 |
| [52] |
D. Li, Z. Tian, W. Tang, et al., Int. J. Mol. Sci. 17 (2016) 935-948. DOI:10.3390/ijms17060935 |
| [53] |
L. Kreja, C. Selig, U. Plappert, W. Nothdurft, Environ. Mol. Mutag. 27 (1996) 39-45. DOI:10.1002/(SICI)1098-2280(1996)27:1<39::AID-EM6>3.0.CO;2-9 |
| [54] |
E.M. Rosen, R. Day, V.K. Singh, Front. Oncol. 4 (2015) 381-396. |
| [55] |
M. Epperly, J. Gretton, S. DeFilippi, et al., Radiat. Res. 155 (2001) 2-14. DOI:10.1667/0033-7587(2001)155[0002:MORICE]2.0.CO;2 |
| [56] |
M. Epperly, V. Kagan, C. Sikora, et al., Int. J. Cancer 96 (2001) 221-231. DOI:10.1002/ijc.1023 |
| [57] |
H. Guo, J. Seixas-Silva, M. Epperly, et al., Radiat. Res. 159 (2003) 361-370. DOI:10.1667/0033-7587(2003)159[0361:PORIOC]2.0.CO;2 |
 2020, Vol. 31
2020, Vol. 31 

